Some users may experience temporary issues accessing parts of the site. Thanks for your patience.
- Office Hours Mon - Fri 9:00 am – 4:00 pm EST
Consequences of these conditions explained by a leading expert, physician and researcher in nasal obstruction, snoring and sleep disordered breathing.
Soroush Zaghi, MD, graduated from Harvard Medical School, completed residency in ENT (Otolaryngology- Head and Neck Surgery) at UCLA, and Sleep Surgery Fellowship at Stanford University. He is active in clinical research with over 60+ peer-reviewed research publications in the fields of neuroscience, head and neck surgery, and sleep-disordered breathing. He recently spoke with Kelley Richardson, our Dawson Academy Airway Curriculum Liaison, to discuss how tongue ties, restricted fascia and mouth breathing can negatively affect sleep, breathing, growth and development.
Kelley Richardson: Many of the dentists who attend our Airway courses are interested in learning more about tongue ties. Would you explain the differences between a functional lingual frenuloplasty versus the traditional type of tongue-tie frenectomy?
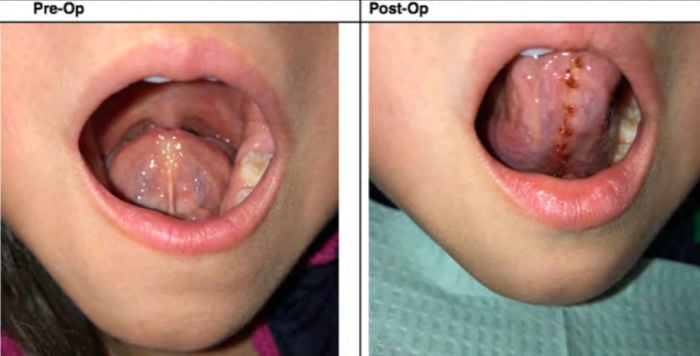
Dr. Soroush Zaghi: Traditionally, you just go in and cut the mucosal frenulum underneath the tongue. The problem with doing that is that in some cases there are still further restrictive fascial or muscular bands that will continue to limit complete mobilization of the tongue. Also, the wounds are left open to heal by secondary intention, so there is a risk that the released tissue can scar back down. Finally, in the traditional technique there is little emphasis on the pre-and post operative care which play in immense role in optimizing the long term result. We contrast that with our functional approach where we work in therapy beforehand to get the tongue adequately toned and strengthened; the release is performed to the appropriate extent necessary to maximize mobility and may include mucosa, fascia, or muscle; and sutures are used to allow healing by primary intention. The major difference is the multidisciplinary protocol that integrates myofunctional therapy and sometimes physical therapy before and after surgery. Myofunctional therapy is like physical therapy for the tongue and is so very important for proper healing and recovery. For example, if you have a knee replacement and you do not do any physical therapy …well, then you’re not going to get a great result. The same principles apply to tongue-tie surgery, where the pre and post-operative therapy will make or break your results.
Kelley Richardson: On a similar topic, would you describe how tongue ties and restricted fascia can affect breathing and posture?
Dr. Soroush Zaghi: Sure. So fascia covers all the muscles in our body. What happens is that when your fascia’s tight because you have a tongue-tie, the tongue is going to be pulled forward with the floor of the mouth. That’s going to cause you to have a tightened fascia system. That fascia coat that we’re in is going to be a little too restrictive, and your body is going to compensate. It’s like you’re walk around in a Spiderman suit that’s too tight. Your shoulders come forward, everything’s constrained. When you release this, everything can open up:
That’s because there’s fascia that goes from the tongue into the chest, all the way down to the feet.
Kelley Richardson: Part of a dentist’s airway screening is to evaluate tonsils. What should dentists know about tonsils and tonsillectomies? Have you found that tonsils can regrow after they have been removed or remodeled? Also, do you find that symptoms that are initially resolved after a tonsillectomy recur over time?
Dr. Soroush Zaghi: Yeah. So there’s different ways of doing tonsillectomy. Some providers actually remove the tonsil, like myself. Other providers don’t remove the tonsil, they just shave it down.
When you shave it down, the advantages of doing that is that it doesn’t hurt as much and there’s less chance of bleeding, but you’re leaving behind some tonsil tissue that can regrow. That’s a partial intracapsular tonsillectomy. I prefer to remove the whole thing. When you do the partial technique, there’s a 3 to 6% chance that it can regrow.
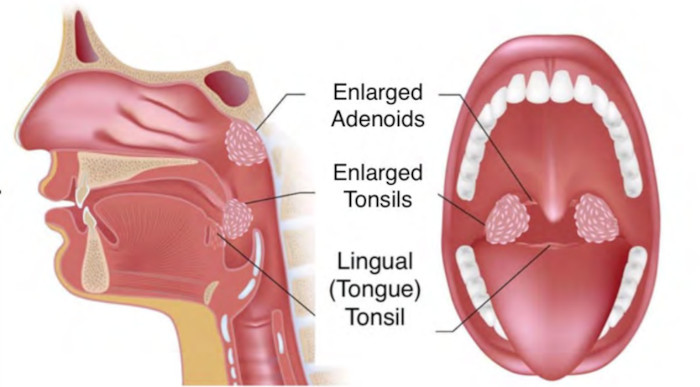 Ultimately, you have to consider why tonsils grow in the first place. It’s because of inflammation in the tonsils, and this inflammation can be propagated because of different reasons.
Ultimately, you have to consider why tonsils grow in the first place. It’s because of inflammation in the tonsils, and this inflammation can be propagated because of different reasons.
Kelley Richardson: What myofunctional or breathing therapy techniques do you recommend for training mouth breathers to breathe strictly through the nose?
Dr. Soroush Zaghi: Dr. Rosalba Courtney has a PhD in breathing therapy, and she’s been advocating for different approaches on this topic. The important thing to consider is that this field is controversial and new. Dr. Courtney talks about the different reasons why someone is not breathing appropriately. It could be engaging muscles because of diaphragm weaknesses. For those patients, she uses a breathing retrainer to actively strengthen the diaphragm. Other times, it’s posture issues that you can work on. For some set of patients in my experience, I have seen people get better with the Buteyko method, specifically patients who are breathing too fast. Not all patients have this problem, but there are some patients that have:
For those people, the concept of breathe less is actually better. For patients with asthma who are pulling in a lot of air, slowing your breathing can be helpful for them. I would say that there’s a role for the different kinds of breathing retraining. You would have to keep a close look and see what the issue is to determine the best method. The underlying thing is that everyone agrees the patient should be breathing through their nose. That’s the commonality among all the different methods.
Kelley Richardson: One of your topics that you will cover in detail at the 2020 International Airway Symposium is pediatric sleep-disordered breathing. Can you briefly describe how a child’s sympathetic nervous system responds to hypopnea (partial airway obstruction) and how it is reflected in behavior?
Dr. Soroush Zaghi: Kids are different than adults in that they’re very resilient. In adults, their arousal threshold is dampened, so it takes a lot more to arouse an adult than a child. For a child, they have a very low tidal volume, so they can’t risk not getting that oxygen. Their breathing tells them that, as soon as the airway narrows, you’ve got to breathe – you’ve got to open up. Adults can tolerate not breathing longer. In a child, maintaining that arousal threshold puts a toll on the body that gets manifested to the adrenal glands’ cortisol increased sympathetic tone. When you’re bathed in this increased adrenaline and cortisol, that’s negatively going to impact:
Cortisol is inversely related to growth hormone release and immune function among other things.
Click here to learn more and to register for our Airway Symposium
ADA CERP is a service of the American Dental Association to assist dental professionals in identifying quality providers of continuing dental education. ADA CERP does not approve or endorse individual courses or instructors, nor does it imply acceptance of credit hours by boards of dentistry.
Concerns or complaints about a CE provider may be directed to the provider or to the Commission for Continuing Education Provider Recognition at ADA.org/CERP.